Psychedelics: entering a new age of addiction therapy*
Bb Janna Lawrence
Gordon McGlothlin is 65 years old and, until recently, he smoked 20 cigarettes a day, a habit he formed when he was just 15 years old. He tried to stop, using nicotine replacement therapy, psychological therapy or going cold turkey. But each time he relapsed. Then, McGlothlin’s friend told him about an advertisement for participants in a clinical trial of a new treatment for tobacco addiction.
So one December morning, McGlothlin walked into the research centre at Johns Hopkins University in Baltimore, Maryland, where he took a small, blue capsule and sat in a room listening to classical music. The idea was that after he walked out of the research centre in the evening he would never smoke another cigarette again. That was almost two years ago and McGlothlin says he is still smoke-free.
McGlothlin was part of a small, proof-of-concept trial using psilocybin to help heavy smokers quit. Psilocybin (pronounced silo-sie-bin) is what makes magic mushrooms psychedelic and, despite its reputation as a recreational drug for hippies, it is showing promise as a therapeutic agent for a number of psychiatric illnesses including addiction, depression and anxiety.
“I think psilocybin gave me the impetus to stay abstinent. It opens up a whole new dimension to your personality. It is almost as though quitting smoking is peripheral during the experience,” says McGlothlin.
In the 1950s, 1960s and early 1970s, psychedelic drugs were extensively researched, with the effects of lysergic acid diethylamide (LSD) being studied in some 40,000 participants. But then LSD was made illegal and research ground to a halt. A retrospective analysis of six trials from the late 60s and early 70s involving 536 patients, published in 2012, found that LSD helped people overcome alcohol addiction and was
“as successful as any treatment since,” says David Nutt, professor of neuropsychopharmacology at Imperial College London and a campaigner for rational drug laws that do not inhibit research.
“We’re talking about one or two doses producing life-long effects.”
Psilocybin and LSD have similar, but not identical, patterns of activity in the brain.
“Psilocybin hits the same primary brain receptor as LSD, called serotonin 2A,” says Matthew Johnson, associate professor of psychiatry and behavioural sciences at Johns Hopkins, who carried out the tobacco addiction trial.
"But, compared with LSD, psilocybin is more appealing to researchers for two reasons: its duration of action is about 6 hours compared with LSD’s 10–12 hours, which makes it more manageable to work with in a clinical setting; and, unlike LSD, it does not have the same strong association with the counterculture of the 1960s," explains Johnson.
“All major drugs of abuse have accepted clinical applications, bar psychedelics. It is really exciting that these drugs could open up novel treatments,” he says, adding that “more and more” scientists are coming into the field.
Johnson recalls how the idea for his smoking cessation study came after looking at historical trials of psychedelics and noticing that their effects could be applicable to a range of addictions, since the reports of experiences were always similar.
“Smoking seemed to be a good place to start.” Johnson continues:
“People may say we are using a sledgehammer for smoking but it is the leading cause of preventable death worldwide and 70% of smokers in the US want to quit.”
Testing time
Johnson and his team enrolled 15 patients in the trial.
“We wanted to demonstrate feasibility of the intervention,” says Johnson. On average the patients had smoked 19 cigarettes a day for 31 years and had six failed attempts to quit behind them. They all received 15 weeks of structured smoking cessation treatment, which included regular sessions of cognitive behavioural therapy (CBT) and administration of psilocybin once each at week 5 and week 7, and optionally also at week 13. It was at the first of these sessions that McGlothlin was given a blue capsule containing pure psilocybin, which takes about 20 minutes to have an effect, and told that this should be his last day smoking. After receiving the treatment, he and the other study participants would stay at the clinic for the whole day, listening to music and being encouraged by the ever-present healthcare professionals to have an introspective experience. At six months follow up, 80% of patients were not smoking.
“The results are not conclusive, but we strongly suspect that it is the psilocybin playing a role, because the quit rates are so much higher than even the best current psychological or pharmacological treatments for tobacco addiction, which are typically around 35%,” says Johnson. Based on the success of the initial trial, he and fellow researchers at Johns Hopkins have now embarked on a phase II randomised controlled trial with 80 participants, which started in October 2014.
Robert West, a health psychologist at University College London who specialises in tobacco addiction, says that the study seems to have been well thought out and conducted, and there is a plausible rationale.
“While probably only a minority of smokers would be interested in using a psychedelic drug to stop smoking, these early results are worth pursuing with a comparative trial,” he says. He adds that
"the proposed mode of action is interesting in that it involves promoting a new outlook on life that may lead to changes in other self-destructive behaviours."
Evidence is mounting that this approach could tackle addiction more generally. A recent study of the psychedelic drug ibogaine found it to be effective at treating addiction to alcohol, cannabis, cocaine and crack. However, Johnson says ibogaine can have cardiovascular side effects and, in comparison, psilocybin is “very safe at a physiological level”.
Psychedelics seem to work in a different way from other treatments for addiction, such as nicotine replacement therapy, which target the same brain receptors as the drug patients are trying to wean themselves off. This difference may be central to why the treatment of addiction is just one of psilocybin’s potential uses. Recently, researchers have started to unpick its effects on brain function — with some striking results. Psilocybin decreases activity in the parts of the brain that are overactive in depression, addiction and ingrained behaviours.
Deactivating cravings
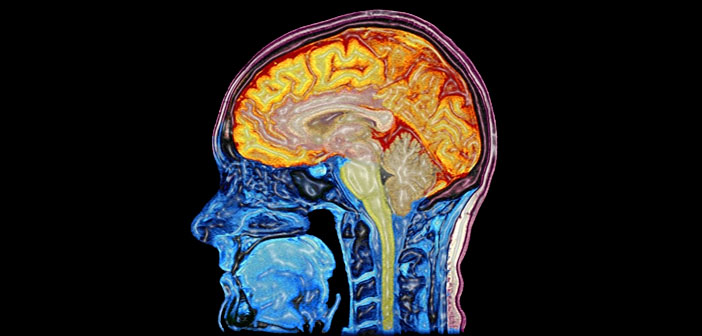
Serotonin 2A receptors, the primary target of psilocybin and other psychedelics, are located in the outer layer of the brain, the cortex. Using functional magnetic resonance imaging (fMRI), Nutt’s team found that stimulation of these receptors by psychedelics decreased rather than increased activity in certain areas of the brain, particularly those in what is known as the default mode network (DMN). The DMN is believed to be involved in introspective thought, our sense of self and our ingrained thought patterns and behaviours.
“During illnesses like depression or addiction, the default mode network in the brain becomes over-engaged with negative thoughts or cravings,” explains Nutt.
"When the DMN ceases to be so over-engaged it “allows people to break free” from these destructive neural patterns," he says.
"Psychedelics make the brain more flexible, with this neuroplasticity potentially underlying their usefulness," says Franz Vollenweider, director at the Neuropsychopharmacology and Brain Imaging Research Unit at the University Hospital of Psychiatry in Zürich, Switzerland. But he emphasises that such agents will probably only work in conjunction with psychological therapy.
His team has discovered that the brain becomes less sensitive to negative information when under the influence of psychedelics.
“In healthy volunteers we found that psilocybin reduces the processing of negative emotional stimuli. This is why we think it can be used in depression,” says Vollenweider.
"Part of this effect could be due to a decrease in reactivity of the amygdala after administration of psilocybin," he says.
The amygdala is deep in the centre of the brain and is responsible for emotions like fear and anxiety. Psilocybin stimulates a specific serotonin receptor which in turn induces a cascade of downstream effects.”
McGlothlin says that because of his treatment with psilocybin, he feels freed from the hold that cigarettes had over him.
“It became non-important, like who cares?” He adds that the experience affected much more than just his addiction to tobacco.
“Psilocybin changed my life. It’s not that I was afraid of dying, but during the experience you come to grips with the fact that life is transient and death a continuation of that process, but that your thoughts persist,” he recalls.
“I had a friend dying of cancer and I think it would have been good for them, it gives tremendous piece of mind, it puts life and death in the right place, it gives you hope.” Indeed, Johnson is one of several researchers who are examining using psilocybin for exactly this purpose.
*From the article here :
Psilocybin, the compound that makes mushrooms magic, is showing promise as a treatment for several psychiatric illnesses.

www.pharmaceutical-journal.com